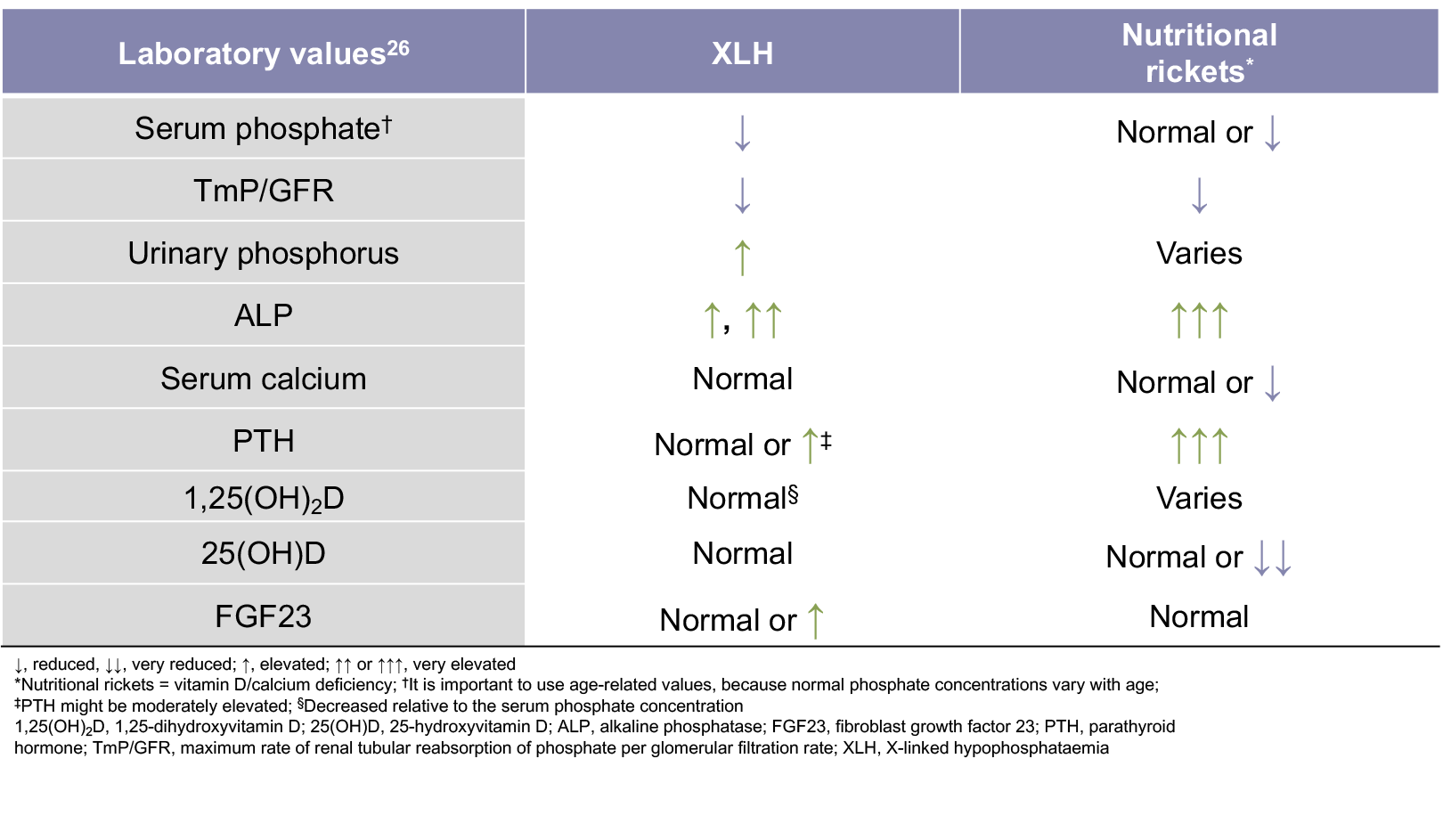
Paediatric assessment
Continually monitor paediatric patients
Since XLH is a chronic, progressive skeletal disorder,1-4 regular assessment is needed from childhood through adulthood to monitor the effects.5 Children should also be asked to identify areas of pain that may not show up during office visits.
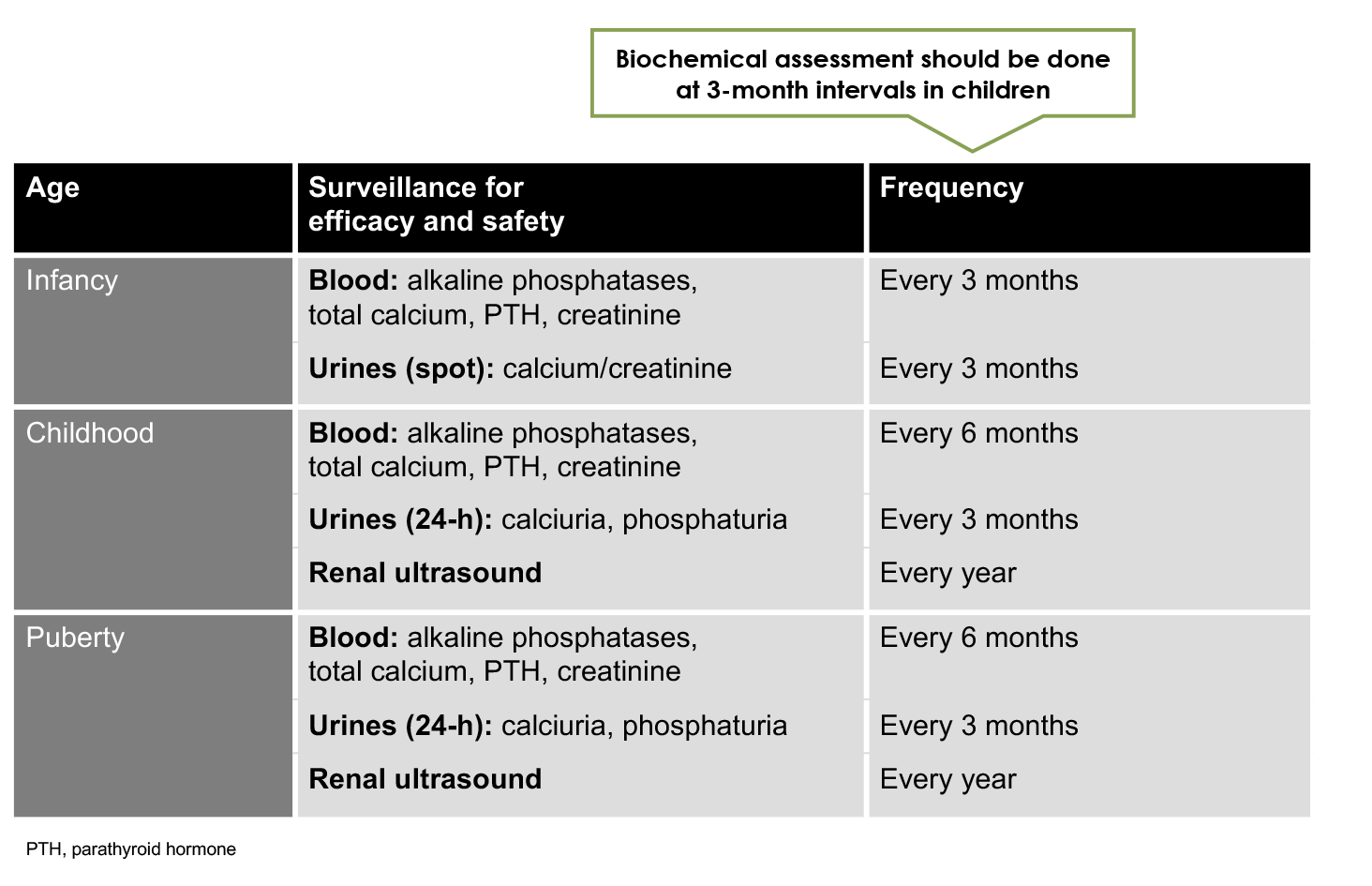
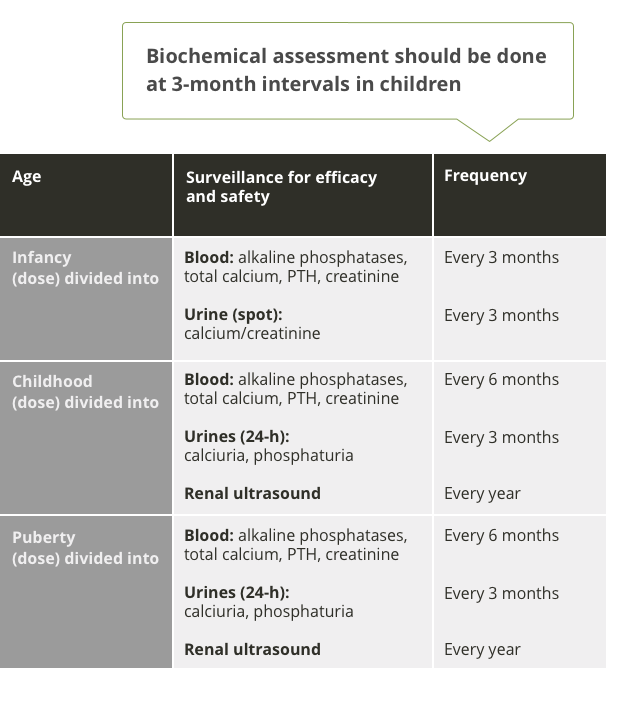
Skeletal assessment for paediatric patients with XLH
XLH is a chronic, progressive disease, with lower limb deformity, loss of growth potential, and body disproportion increasing with age. Children should be routinely assessed for safety and response to medical treatment.6,7
Anthropometric measurements
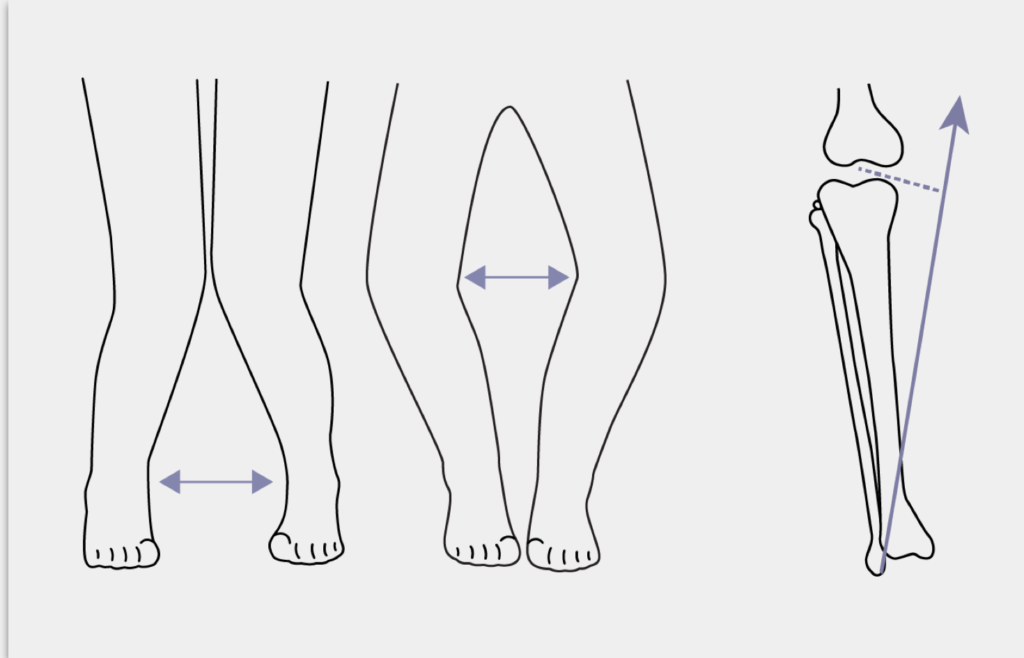
Tibiofemoral angle
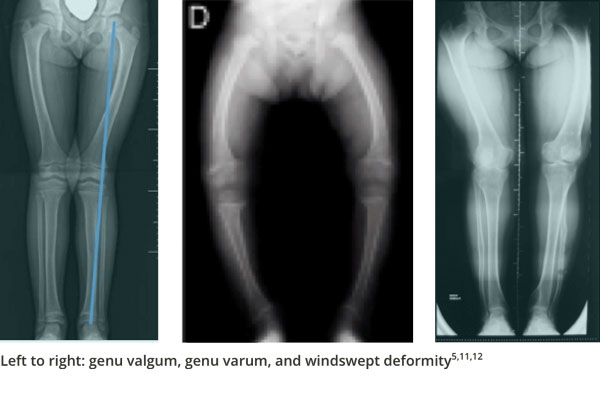
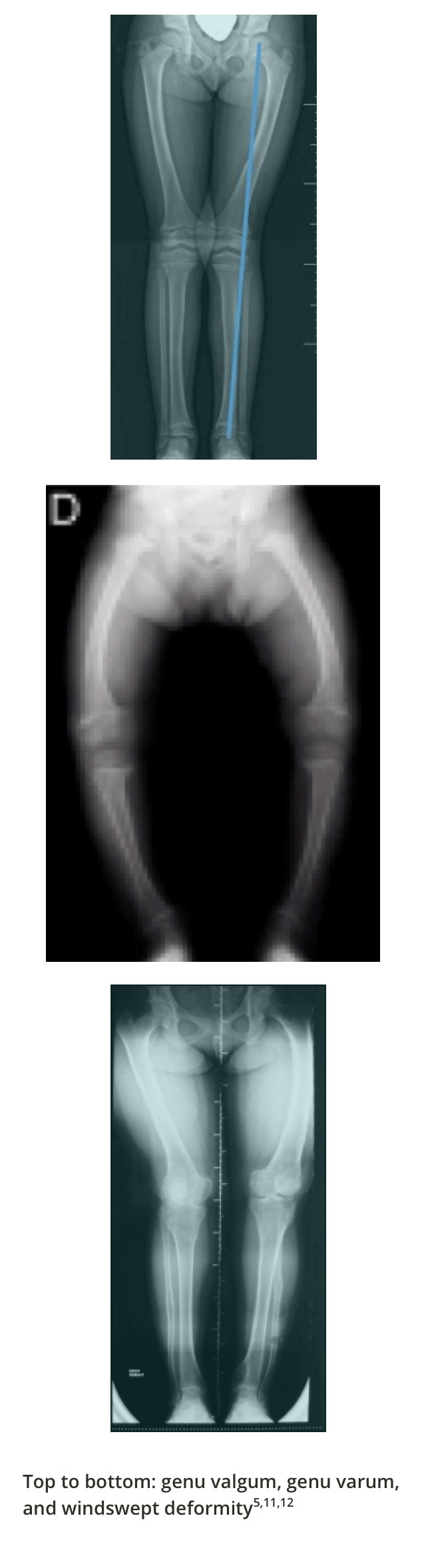
The tibiofemoral angle can be clinically assessed by the intercondylar and intermalleolar distances. A variation becomes a deformity when the amount of deviation from normal for that particular age is >2 SD. Response to conventional therapy is defined as a 1-cm decrease in genu valgum or genu varum every 6 months.5,10
Age-related growth and proportion evaluation is comprised of different assessments: standing and sitting height, and arm and leg length.9
Leg length should be measured as standing height versus
sitting height.9
Recumbent Length
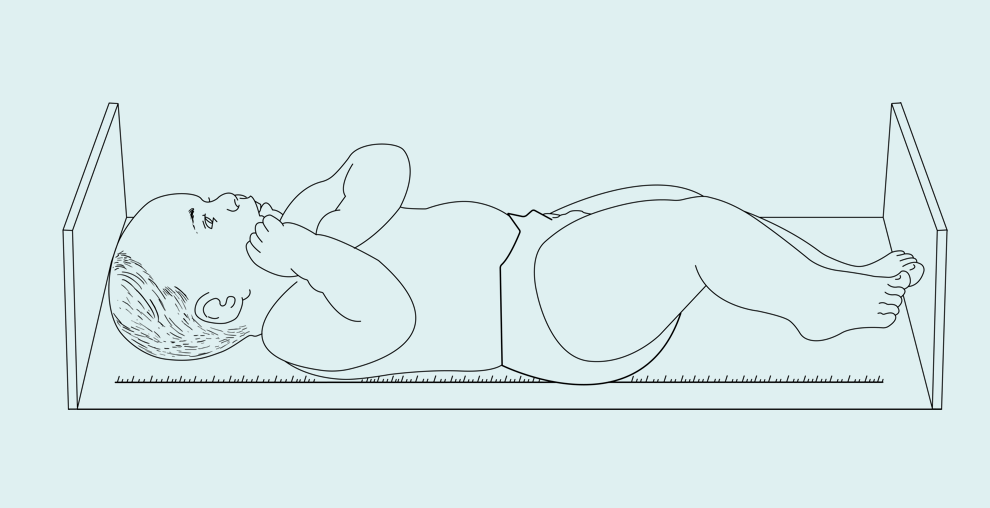
Two people are required to measure recumbent length. The patient’s head is positioned on a fixed headboard, while the feet are positioned and the footboard adjusted for measurement.
The child is placed supine on the infant board with buttocks and shoulder blades in contact with the board. The child should be measured with minimal clothing. The Frankfort horizontal plane13 should be parallel to the head and foot boards. The patient’s head should be up and their eyes facing forward. Gentle pressure should be applied to the legs to prevent the knees from flexing, while the footboard is adjusted until it rests firmly against the child’s heels.
Growth
Children with XLH generally show disproportionate growth, so regular measurement and assessment are important.9
Height-for-age Z-score: Growth Z-scores reflect the number of standard deviations from age- and sex-matched normal mean values.14
- Z-scores are based on standard growth references collected from normal children
- The WHO recommends cutoff Z-score values of ±2 to define abnormal growth
- Short stature is defined as height-for-age Z-scores <–2 for individuals of the same sex

Rickets often causes lower-extremity deformity and loss of growth potential.6
Because of open epiphyses, patients present a significant risk of recurrent bowing at the level of osteotomy or secondary to adjacent epiphysiodesis.5
Quality of life and physical function for paediatric patients with XLH
Several different tools are available to assess quality of life and physical function
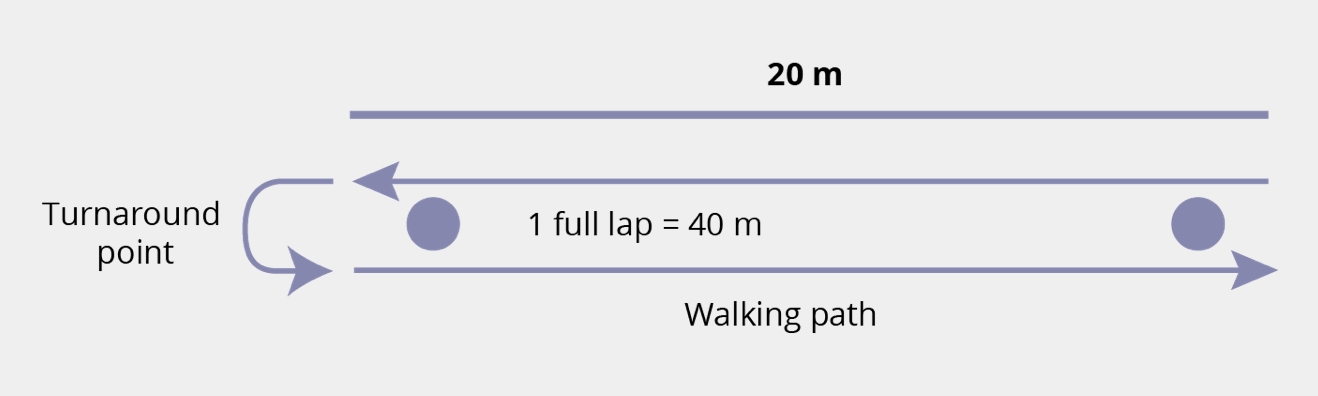
The 6MWT is a practical, simple test that measures how far a patient can walk in 6 minutes on a flat, hard surface.
A parent-completed questionnaire to assess overall health, pain and ability to participate in normal daily activities, as well as in more vigorous activities associated with young people.
PROMIS (Patient-Reported Outcomes Measurement Information System)17
PROMIS was developed by the NIH and uses domain-specific measures to assess physical, mental, and social health.
The SF-10 for Children™ is a short-form survey that contains items adapted from the CHQ (Child Health Questionnaire) and scored to produce physical (PHS) and psychosocial health (PSS) summary scores.
Pain intensity is a self-reported measure of pain intensity developed for children.
Measuring
The TmP/GFR is the ratio of renal tubular maximum reabsorption of phosphate (TmP) to glomerular filtration rate (GFR).6,20-25